Content
According to statistical data, cervical ectopia of the cervix can be called the most common condition, which does not always indicate pathology. The frequent occurrence of cervical ectopia is due to the mechanism of its occurrence. Often this condition of the cervix is asymptomatic and is detected randomly at an appointment with a gynecologist.
Concept of cervical condition
Cervical ectopia implies localization of the epithelium of the cervical canal on the cervix. Ectopia literally means "outside". Regarding the cervix, gynecologists use the concept of cervical ectopia when the boundaries of the columnar epithelium are displaced. Thus, some part of the epithelium of the cervical canal comes out. Cervical ectopia is visualized during a gynecological examination, as it is an area of mucous membrane that differs in color and texture.
The cervix has its own structural features. First of all, this part of the uterus is not considered as a separate organ of the reproductive system. The cervix functions as the lower narrow section of the uterus, located between the body of the organ and the vagina. This localization provides a unique protection mechanism, since the cervix is a barrier to infection.
It is known that the uterine cavity is sterile, and the vagina is inhabited by a variety of microorganisms that can cause an inflammatory process. The uterine body communicates with the vagina through the cervical canal, which connects these areas to each other.
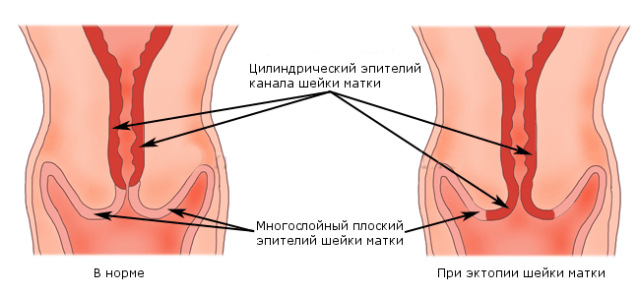
The cervical canal is quite narrow, its length does not exceed a few centimeters. It is covered with single-layer columnar epithelium, which gives the mucosal surface a red tint and some velvety feel. The cylindrical canal, like the cervix as a whole, takes part in childbirth. It contains numerous folds that allow it to stretch. Thanks to the folds, the cervical canal has the appearance of a spindle.
In the submucosal layer of the cervical canal there are numerous glands that continuously produce mucus. Mucus production varies depending on the phase of the cycle and the influence of estrogen hormones. The mucous secretion fills the cervical canal like a plug, which prevents infection from entering the uterine cavity. In addition, the secretion has bactericidal properties. Thus, protection is provided both by the mucus and the narrowness of the channel itself.
The upper edge of the cervical canal is called the internal os, and the lower edge is called the external os. These are two physiological constrictions that also provide a defense mechanism. Inside the external pharynx there is a transition region or transformation zone connecting the epithelium of the cervical canal and the vaginal part of the uterus.
There are two sections in the structure of the cervix:
- vaginal visible, protruding into the vagina;
- supravaginal invisible, adjacent to the uterine body.
The vaginal part of the cervix is examined in speculum during a gynecological examination. It is covered with squamous stratified epithelium and appears as a uniform, pale pink mucosa.
Cervical ectopia is considered the most common condition of the cervix in global gynecological practice. It is detected in 40% of women, and among women with gynecological diseases, cervical ectopia is detected in every second case.
Many women believe that cervical ectopia occurs only in connection with sexual activity. However, it should be taken into account that a gynecological examination in virgins is difficult. It has been proven that cervical ectopia can be congenital and hormone-dependent.
Cervical ectopia can be either a pathology or a normal physiological condition. In particular, congenital and uncomplicated ectopia are considered a normal variant and do not require treatment, but only observation. Hormonal changes during pregnancy can also provoke the development of a defect in the cervix. Most cases of cervical ectopia occur in women who have not completed their reproductive function.
The disease is considered complicated form, manifested by symptoms.
Cervical ectopia of the cervix is not an erosion. This is due to the fact that erosion always implies a wound surface, while ectopia is not accompanied by damage to the epithelium.
For quite a long time, cervical ectopia was considered as a precancerous process. That is why, when this condition of the cervix was identified, appropriate treatment was mandatory. Currently, this defect is considered a benign condition.
Gynecologists say that there are many factors and causes for the appearance of cervical ectopia. The main causes of the defect are damage to the mucous membrane by infections, as well as mechanical damage. In some cases, the occurrence of a benign condition is associated with a combination of various unfavorable factors.
In general, the defect on the cervix progresses latently. However, the presence of manifestations may be related to the size of the spot. For example, large cervical ectopia may be accompanied by contact discharge during sexual intercourse or gynecological examinations. Sometimes there is the appearance of leucorrhoea and an increase in leukocytes in the smear. However, complaints with ectopia are often associated with concomitant gynecological diseases, which are the cause of symptoms.
Adverse effects on the cervical mucosa do not always lead to the appearance of an epithelial defect. That is why it is not entirely correct to name with certain precision the reasons leading to the occurrence of cervical ectopia.
Determination of cervical ectopia occurs during a visual examination of the cervix. The gynecologist visualizes a red spot against the background of pale pink smooth epithelium, which has different sizes and shapes. In addition, the cylindrical epithelium causes velvety appearance.
With a complicated form, there is a need for mandatory treatment. As a rule, treatment involves destruction of the lesion with electric current, radio waves, laser, chemical solutions, liquid nitrogen, and argon. The optimal tactic for removing a defect is considered to be radio wave exposure.
Causes
The surface of the cervix and vagina are covered with three layers of squamous cells, while the cervical canal is lined with single-layer cylindrical cells. Typically, the cervical defect is located inside the external os in the so-called transformation zone, which is invisible during examination.
When columnar epithelium slips from the area of the cervical canal, the transformation zone gets mixed up. This is why cervical ectopia becomes visible.
The mechanisms of defect formation have not been sufficiently studied. In particular, the congenital type of defect is formed due to impaired differentiation of squamous and columnar epithelium. This occurs if differentiation occurs before the formation of other parts of the cervix. A congenital defect is regarded as a variant of the norm. Sometimes a congenital defect of a physiological nature is associated with estrogen deficiency, which affects the developing tissues of the reproductive system. When puberty ends, the ovaries are fully functional. This helps to move the border to its proper place. Thus, the ectopia disappears. Therefore, a birth defect is the only type that can regress on its own.
A birth defect is considered to be a temporary physiological condition. The acquired variety is the result of exposure to unfavorable factors on the cervix.

Gynecologists identify the following causes and factors that predispose to the appearance of acquired cervical ectopia.
- Infectious process. Often the cause of the defect is an inflammatory process caused by sexually transmitted infections. As a rule, both the vagina and the cervix are involved in the inflammatory process. This is due to the close anatomical and functional connection of the tissues. Inflammation can be caused by both conditionally pathogenic and specific flora. Specific microorganisms have an aggressive effect on the cervix. Erosion occurs on the surface of the cervix. If erosion does not heal correctly, the formation of pseudo-erosion or acquired ectopia is observed.
- Promiscuous sexual intercourse and lack of barrier contraception. These factors contribute to sexually transmitted infections, unwanted pregnancy, and infertility.
- Frequent mechanical damage to the cervical tissue. The causes of cervical ectopia are abortions, repeated surgical procedures, and difficult childbirth.
- Hormonal disorders. Hormonal dysfunction negatively affects the condition of the reproductive organs.
- Early sexual activity and childbirth. These factors contribute to traumatization of cervical tissue, which is immature. In addition, insufficient hormonal regulation also predisposes to the occurrence of the defect.
Sometimes the appearance of cervical ectopia is multifactorial.
Symptoms
Typically, a cervical defect does not have specific signs. In most cases, the emerging clinical picture is associated with the presence of concomitant gynecological diseases of the inflammatory and hormonal nature.
If uncomplicated ectopia occurs on the cervix, there are no manifestations. Sometimes patients complain of abundant mucous discharge, which is the result of the functioning of the glands of the columnar epithelium. Contact discharge may appear due to trauma to the ectopic site. An increased number of leukocytes may be detected in smears.
The defect is detected by chance during an examination by a gynecologist. It is impossible to determine by the appearance of the spot how long ectopia has existed on the cervix. It is likely that it is congenital in nature and is associated with impaired differentiation of tissues of multilayered squamous and single-layer cylindrical epithelium. It is believed that most birth defects disappear by the time sexual activity begins. That is why the number of diagnosed congenital ectopias is small.
A significant number of cervical ectopias are acquired. In addition, in 80% of cases such defects are complicated. Simultaneously with ectopia, an inflammatory process is present, which determines the presence of characteristic symptoms. The clinical picture of complicated ectopia includes a variety of signs:
- pathological discharge;
- itching of the genitals;
- burning when urinating;
- pain in the lower abdomen.
If the defect is of a significant size, contact discharge often appears. Postpartum ectopia has no specific symptoms. Its manifestations can be disguised as postpartum symptoms. The diagnosis is made during a routine examination.
Cervical ectopia does not affect reproductive and menstrual functions. If cycle disorders or infertility occur, ectopia may be associated with hormonal disorders.
Varieties
Cervical ectopia implies a connection between the defect and the cervical canal. Often it is acquired. For a long time, experts believed that the appearance of the defect was associated with the desire of the cylindrical epithelium to close the ulcer formed as a result of damage to the mucous membrane. Thus, cervical ectopia was a unique way of restoring tissue due to cylindrical rather than flat epithelium.
In modern gynecology, the theory of the connection between erosion and ectopia is often refuted. Many scientists are of the opinion that cervical ectopia has hormonal causes. Thus, the cause of the spot may be a hormonal imbalance.
There are several types of ectopia, which are distinguished according to the nature of the growth of cylindrical cells.
- Glandular. The columnar epithelium contains glands. Once on the surface of the neck, this species retains its properties. It is known that the glandular variety is distinguished by a large number of glandular structures and signs of inflammatory infiltration.
- Papillary or papillary. With this form, the columnar epithelium grows in the form of papillae. In turn, each papilla has a vascular terminal loop.
- Healing or epidermising. Single islands of squamous epithelium are observed at the location of the cylindrical tissue.
When prescribing treatment Determining the type of defect is not fundamental.
Diagnosis and treatment
Cervical ectopia can be detected during a gynecological examination. Doctors examine the cervix in a speculum and identify a reddish area that stands out against the background of healthy mucous membrane. The spot can have different sizes and shapes, usually located near the cervical canal.

In the presence of concomitant infection, pathological discharge, edema and hyperemia are observed. Complicated ectopia looks more pronounced. Sometimes it becomes covered with a purulent coating. With concomitant inflammation, it is difficult to determine the size of the spot due to swelling.
When a defect is detected, a colposcopy becomes necessary. This is due to the fact that various pathologies, including cervical cancer, can be disguised as cervical ectopia. Using a colposcope, the doctor carefully examines the external characteristics of the spot thanks to the presence of a lighting and magnifying system of the device.
In order to determine the size and boundaries of the spot, an extended colposcopy is performed. The area of the cervix is treated with a solution of acetic acid. At the same time, the vessels contract, and the defect changes color and texture. The gynecologist visualizes glassy growths in the form of grapes of columnar epithelium.
Then a test is carried out with Lugol's solution. Iodine reacts with glycogen in the squamous epithelium, which is accompanied by a brown color. Areas with columnar epithelium do not darken.
When performing a cytological examination, leukocytes, erythrocytes and cells of multilayer and single-layer epithelium are detected in the smear. The following conclusions are possible.
- Uncomplicated ectopia: without features, proliferation of columnar epithelium, cytogram of endocervicosis.
- Complicated ectopia: cytogram of inflammation.
When a complicated variant of the defect is identified, the list of diagnostic measures expands. Experts recommend doing:
- flora smear;
- bacterial sowing;
- PCR for detection of sexually transmitted infections.
If there are cycle disorders and infertility, a study is prescribed to determine the hormonal status, as well as an ultrasound.
Cervical ectopia is not dangerous from the point of view of the development of a malignant tumor. However, sometimes cervical cancer masquerades as a benign defect. If atypical cells are detected during a cytological examination, a histological diagnosis should be performed, which is possible through a biopsy of the defect tissue and curettage of the cervical canal.
Treatment is prescribed after a complete diagnosis. Uncomplicated and congenital ectopia cannot be treated.
The choice of the optimal treatment method determines its effectiveness and is the prevention of relapse. All defect elimination methods used in gynecological practice are effective.
Destruction of the pathological area is not carried out in the presence of an inflammatory process. This is due to the fact that the infection will interfere with the regeneration processes. When genital infections and inflammation are detected, antibacterial therapy is carried out. Cauterization is possible only after treatment has been carried out and the absence of infectious pathogens has been confirmed.

Cauterization or destruction of pathological foci is carried out using several techniques. Each tactic has both positive and negative sides.
In modern gynecology, the following tactics for the treatment of cervical ectopia are successfully used.
- Diathermocoagulation. Cauterization with electric current or electrocoagulation has been used since the beginning of the last century. This is the very first way to eliminate pathological areas from the surface of the cervix. The method is quite painful and traumatic. Nevertheless, diathermocoagulation is highly effective. In addition, the technique is simple and does not take long. Equipment for diathermocoagulation is located in every gynecological medical institution. After cauterization, a scab forms, which comes off after a few days, accompanied by slight brown discharge. After the manipulation, a scar remains on the cervix. Complications often develop, for example, fusion of the cervical canal and infection. The method is not recommended for nulliparous girls.
- Cryodestruction. This is the effect of liquid nitrogen on the cervix, which is supplied through a cryoprobe. Compared to electrocoagulation, this technique is less traumatic. The cells of the spot crystallize and destroy. After the manipulation, abundant liquid discharge is observed for two months. The method is effective only with minor damage to the cervix.
- Laser coagulation. Exposure to the laser leads to the evaporation of pathological cells. During the treatment process, healthy tissue is practically not injured. However, there is a risk of seeding healthy areas with cells that have undergone evaporation.
- Radio wave destruction. Today this is the most effective and gentle treatment method. In the process of removing the defect, the vessels are coagulated and the wound is sterilized. This prevents bleeding and infection. The technique is recommended, including for nulliparous patients.
With an adequate choice of treatment method, you can count on a complete cure.
Women of reproductive age, as well as young girls, often hear from a gynecologist a diagnosis of cervical ectopia. Most often, post-Soviet doctors suggest getting rid of this condition as soon as possible. Let's discuss how the procedure for cauterizing erosion corresponds to the medical practice of developed countries.
When examining the patient on the chair, the gynecologist can see that the outer surface of the cervix is red. Typically, such changes are observed around the pharynx covering the canal. Redness may vary in degree. For some, the entire surface of the cervix changes, while for others only a small area.
In gynecology, there are about twenty pathologies in which the doctor sees hyperemia during examination. If the doctor has little experience, he will immediately diagnose erosion and suggest conservative therapy to begin with. If it doesn’t help, and it can’t be otherwise, then they move on to heavy artillery - removal by radio waves or another similar method. Let us note right away that ectopia does not require treatment of the cervix. We'll explain why below.
True erosion
With this disease, the mucous membrane is injured if it is exposed to a caustic substance such as soap, alkali, acid, or due to the use of some kind of medication. In addition, a woman can injure the surface epithelium with tampons. Intrauterine devices to protect against unwanted pregnancy, as well as the diaphragm, can cause damage to the mucosa. During medical manipulations using instruments, it is possible that true erosion will occur.
Upon examination, the gynecologist will find a swollen area with a loose red texture. Usually there will be bleeding as from any wound. It will intensify during sexual intercourse. Most often, such erosion does not require treatment. It heals on its own if the traumatic impact has stopped. Some doctors diagnose erosion if the patient has cervicitis, ectropion and other diseases.
During pregnancy, cervical ectopia is also not uncommon. In young girls who have not yet given birth to a child, ectopia is often detected. By mistake, the doctor calls what he saw ectropion.
Differences
Ectopia is an abnormal anatomical location of an organ or tissue within another organ or organism. Ectropion is the turning out of what should be inside. It turns out that this concept explains the mechanism of the appearance of ectopia.
Source: diagnosis-online.ru
The cervix is lined with mucous membrane, which comes out at certain points in a woman’s life. This happens during puberty or when taking hormonal contraception. Pregnancy and cervical ectopia also overlap quite often.
Considering the fact that the protruding section of the integumentary epithelium is single-layered, blood vessels are visible through it. Therefore, the doctor will see redness at the site of ectopia.
Many doctors may call ectopia pseudoerosion. There is absolutely no point in treating her. And even dangerous, because surgical methods are used that injure the neck. Very rarely, intervention is not necessary if a woman feels discomfort and has red discharge from the genital tract.
As already mentioned, inflammatory pathologies are not cervical ectopia, although they may look the same. With viral cervicitis, hyperemia is detected on the entire surface of the cervix, which the doctor interprets as extensive erosion, frightening the patient.
When a gynecologist diagnoses you with erosion, ask him what exactly he means by it. Sometimes a specialist will start to scare a woman that if nothing is done, the ectopia will degenerate into cancer. It is not true. On the contrary, in this condition the mucous membrane is accessible for examination, and is not hidden inside.
As soon as the doctor tells you that the cervix is hyperemic, then you need to begin the examination. The gynecologist usually does this. First, a cytological smear is taken to study the changed cells. The cervix must be examined using a colposcope - a special microscope.
It is very important to exclude inflammation. No treatment can be started if infectious agents are found in the discharge. If you want to see what cervical ectopia looks like, photos from the Internet will help you.
When in doubt, the doctor may take a biopsy of the changed area. Some specialists do not warn the patient about this and take the material rather roughly. This causes unpleasant pain that the woman was not prepared for. There is also a nuance that during inflammation it is contraindicated to take tissue for analysis. After the biopsy, you should not have sex for at least 7 days, otherwise there is a high risk of infection of the affected area.
Cervical ectopia during pregnancy - what is it? Only a real specialist knows. During this period, he certainly will not subject the woman to tests called a biopsy. Against the background of decreased immunity, inflammation could begin. And then the pregnant woman, together with the gynecologist observing her, decide which remedy is best to use so as not to harm the unborn child.
Let's see why histological examination is necessary.
When tissue changes occur, it is necessary to exclude dysplasia, a precancerous condition of the cervix. Many specialists, when they see extensive erosion, begin to frighten their patients. But it's not that simple. Most often, it is the outwardly healthy mucosa that may contain cancer cells. Just the same, cytology allows us to exclude a malignant process.
Cancer
Cervical ectopia has various and often completely harmless causes. If we talk about statistics, cervical cancer is a rather rare pathology in the countries of the former Soviet Union. And yet gynecologists regularly intimidate poor patients. Why is that?
The thing is that each area has its own prevalence of one or another pathology. Thus, in the United States, one woman out of 21,000 of all representatives of the fair sex gets cervical cancer.
A disease is called rare if it is diagnosed only once a year among 20-200 thousand patients. Therefore, a doctor who sees you in a regular clinic, and not in an oncology clinic, will honestly answer you that he was able to confirm no more than one oncological pathology over the past 1-3 years.
So scaring patients with untreated erosion is a common practice in order to carry out an expensive cauterization procedure. Cervical ectopia itself is not a precancerous condition.
There is only one pathology that is classified as precancerous. This is dysplasia. And then, only its severe form.
Dysplasia
The diagnosis of dysplasia is made after a laboratory analysis to evaluate the nature of the cells of the mucous membrane of the neck. Even a healthy organ can have dysplasia areas. Note that not every dysplasia will turn into cancer. And it is also not always necessary to treat this condition of the mucous membrane.
Dysplasia, depending on the depth of penetration into the tissue, can be:
- light;
- moderate;
- heavy.
If you believe American statistics recording cases of dysplasia, then a mild degree is recorded in 3.8% of cases, and moderate and severe is no more than 0.8%. As for cancer, cytology detects it in 0.1% of women.
Cervical ectopia, a photo of which may frighten particularly impressionable people, is often mistaken for dysplasia. In this case, you need to look for a gynecologist who knows how to distinguish normal from pathology.
Despite the fact that medicine is available in many countries today, cytological smears are not practiced everywhere. In addition, they are often taken incorrectly, which leads to false results in both directions - negative and positive.
Approximately 3% of deviations from the norm in 90% of cases, mild forms of dysplasia go away on their own. The remaining 10% can progress and lead to severe or moderate pathologies.
As for moderate dysplasia, it successfully disappears without treatment in 70% of cases and only 20% progress further. The data were checked multiple times based on the medical records of women from different countries. For those who have a mild degree of dysplasia, observation with regular cystological examination every six months is indicated. There is no point in rushing to treat dysplasia. Rebirth, if possible, lasts about 15 years.
Cervical ectopia most often has traumatic causes. For example, childbirth. Dysplasia can be caused by the following factors:
- more than two or three births in a short period of time;
- lack of vitamin A, C and beta-carotene in the diet;
- long-term use of oral contraception (more than five years);
- serious disruption of the immune system (HIV);
- burdened heredity in terms of malignant processes of the reproductive system;
- infections acquired through sexual contact;
- human papillomavirus (HPV);
- smoking, both active and passive;
- multiple sexual relations;
- poor living conditions;
- early first sexual intercourse before 16 years of age.
The same factors influence the occurrence of cervical cancer.
It is important to know that HPV is a virus that can cause both dysplasia and cancer. As for other viruses (herpes, cytomegalovirus, Epstein-Barr) and bacteria (diplococcus, chlamydia), scientists were unable to link them with changes in the cervix.
Treatment of the cervix, the ectopia of which is either weakly or quite strongly expressed, is not associated with any viruses. But severe and moderate dysplasias are more common in patients who simultaneously have several viruses in their bodies - HPV and herpes type 7.
However, in the presence of human papillomavirus in combination with mild dysplasia, surgical treatment is not indicated. In some countries it is even strictly prohibited. Only in the case of a severe or moderate stage can we talk about this.
Treatment
With diseases such as gonorrhea or chlamydia, it is not the outside of the cervix that is affected, but its canal. Mycoplasma and Ureaplasma are safe for women because their main target is the male urethra. It will not be possible to examine vaginal secretion to identify the pathogen at one time, since each microorganism is diagnosed under certain conditions.
It happens that the result of a cytological analysis does not reveal dysplasia. Then you need to perform a colposcopy - examine the suspicious area under a microscope. It is very important that the results of both the analysis and colposcopy coincide. Otherwise, another examination is needed in three months.
Pregnancy and cervical ectopia, as we have already mentioned, do not interfere with each other. In the case of dysplasia, a more detailed examination is usually prescribed after birth.
If the doctor suspects a severe degree of dysplasia, then only a biopsy is indicated. In developed countries, surgery is prohibited if the results of several examinations are different.
Today medicine offers several treatment options:
Chemical cauterization. This method will help cope only with mild dysplasia. In other cases, the effect will be zero. The most commonly used drugs are solcogin, vagotide and others.
Surgical intervention. This includes three options for influencing the cervix: diathermocoagulation - cauterization using electric current;
- Cryodestruction - freezing with nitrogen, which is in a liquid state;
vaporization or excision of the neck with a laser. - Very rarely, conization is used, in which part of the cervix is removed with a scalpel. This requires very serious indications, as does the removal of the entire cervix.
All methods have both negative and positive sides. Only a specialist should choose, taking into account the characteristics of each specific case.
So, if the patient suffers from HPV infection, then the optimal treatment for the cervix (ectopia is not considered, only severe dysplasia) is diathermocoagulation or laser excision. The operation is performed in the first phase of the menstrual cycle. Increasing estrogen levels promotes epithelial growth, so healing will occur faster. Surgery has contraindications and a risk of complications. The gynecologist should give you this information.
Below we suggest that you familiarize yourself with when the operation is impossible:
- during pregnancy, cervical ectopia and dysplasia are not treated;
- survey results vary;
- the pelvic organs are under attack from an infectious process;
- if you suspect cancer;
- the affected area is too large.
In fact, there are many more contraindications, which your doctor should tell you.
Recovery
The gynecologist is obliged to tell you what you will encounter after the operation.
Most often these will be the following conditions:
- nagging pain in the lower abdomen for 2 days;
- spotting for about four weeks.
To get rid of pain, you can take painkillers. Do not lift heavy objects during recovery. Sexual relations, tampons and douching are prohibited. Any factors that injure the mucous membrane can increase bleeding or cause an inflammatory process due to infection.
Antibiotics are not indicated for normal healing. Some doctors use hormonal contraceptives to delay the onset of menstruation to prevent endometriosis. Research does not support the effectiveness of these measures.
Pregnancy
As soon as the mucous membrane is completely restored, you can plan conception. This usually takes about 10 days. A cytology smear will be reliable in 3-4 months.
After surgery, some patients experience prolonged healing—about six months. And this is also considered the norm. That is why the result is assessed only after 6 months, not earlier.
Not all doctors warn women about what consequences await them after cauterization or excision of the affected area. It is especially important to assess all risks if a woman is planning a pregnancy.
List of possible complications:
- narrowing of the cervical canal, which leads to infertility;
- reduction of mucous secretion;
- the cervix becomes defective, therefore it does not fully perform its functions;
- fallopian tube dysfunction may occur due to ascending infections;
- deformation of the cervix due to the formation of scar tissue;
- if the examination is inaccurate, cancer cells may continue to develop;
- menstrual irregularities;
- exacerbation of chronic pathologies of the pelvic organs;
- premature birth;
- early rupture of the membranes (usually this happens after diathermoelectrocoagulation).
The latter complication is quite dangerous, therefore, when performing any manipulations on the cervix, the doctor must find out whether the woman plans to give birth to children in the near future.
During pregnancy, cervical ectopia does not require treatment at all. If a specialist detects changes in the mucous membrane, it is necessary to make sure that there are no cancer cells. When diagnosed with dysplasia, it is important to check with your doctor what degree you have. With a mild degree, you can become pregnant, but the examination should be repeated after six months or earlier - after three months.
For moderate dysplasia, it is necessary to repeat cytology and colposcopy after three months. For severe cervical dysplastic changes, discuss a plan of action with your doctor, taking into account that you want to have a baby in the foreseeable future.
As you can see, radical treatment of the cervix is a last resort measure that should be used very rarely. This is especially true for young girls with a normal cytological smear.
Cervical ectopia, no matter what size it is, is a physiological norm and does not require therapy. An examination once every six months will allow you to maintain your health and timely notice changes in the reproductive organ, which is so important for women.
Often, cervical erosion refers to ectopia (pseudo-erosion), which refers to underlying benign diseases of the cervix. This is exactly what will be discussed in the article.
When they talk about cervical erosion, they mean a defect in the mucous membrane of the vaginal part of the cervix. This may be an ulcer or ulceration, but most often it is the replacement of one type of epithelium by another.
Erosion usually develops in women of childbearing age, that is, up to about 40 years of age.
Kinds
There are three types of cervical erosion:
Congenital erosion.
It is diagnosed in girls of adolescence and adolescence; it looks like a bright red formation around the external pharynx.
True erosion.
It is a defect (ulceration) of the epithelium that covers the visible part of the cervix. This type of erosion does not exist for long, a maximum of 2 weeks, after which it either disappears on its own or turns into pseudo-erosion of the cervix. True erosion looks like a bright red spot around the external pharynx, reaching about a centimeter in diameter and having clearly defined edges.
Pseudo-erosion or ectopia.
It is formed by columnar epithelium, which should line the cervical canal, while the vaginal part of the cervix is normally covered by stratified squamous epithelium. In other words, one epithelium is replaced by another.
Causes
The reasons that lead to the occurrence of cervical pseudo-erosion are numerous and varied. These include:
- cervical trauma (damage to the cervix during abortion, childbirth or rough douching);
- early sexual activity or, conversely, late onset;
- promiscuous sexual intercourse;
- sexual infections;
- diseases of the cervix (cervicitis, cervical deformation and others);
- hormonal imbalance and endocrine pathology;
- weakened body defenses;
- childbirth in adolescence (up to 16 years);
- genetic predisposition;
- non-compliance with the rules of personal hygiene or excessive enthusiasm for it (deep washing).
Symptoms of cervical ectopia
Often, cervical erosion is asymptomatic, that is, the disease does not manifest itself in any way. As a rule, it is an incidental finding during a gynecological examination, which is why you should visit a gynecologist twice a year.
However, in some cases, cervical ectopia makes itself felt. Firstly, there may be an increase in vaginal leucorrhoea, which usually does not have an unpleasant odor, and when an infection, often accompanying pseudo-erosion, occurs, the discharge changes its character: it becomes cheesy, greenish-purulent, etc. Accordingly, the smell becomes different.
Secondly, some women report contact bleeding (for example, after intercourse or douching). They are not abundant, bright red in color, and disappear quickly.
Thirdly, patients may complain of minor or moderate pain in the lower abdomen.
When examined in the mirrors, the doctor immediately sees an uncharacteristic red spot around the external pharynx, which leads him to think about cervical ectopia.
Diagnostics
It is necessary to carry out a differential diagnosis of cervical ectopia so as not to confuse it with ectropion, true erosion, erythroplakia and cervicitis. If a woman is pregnant, it is necessary to distinguish bloody contact discharge from the threat of miscarriage.
The following methods for diagnosing ectopia are used:
- examination of the vaginal part of the cervix in a speculum and taking a smear from the cervical canal and vaginal part of the cervix for oncocytology (atypical cells);
- colposcopy with samples;
- targeted biopsy (under the control of a colposcope, a small piece of tissue is taken from the most suspicious area);
- examination for all (preferably) infections that are sexually transmitted (human papillomavirus, chlamydia, ureaplasma, herpes infection and others);
- blood for syphilis (ectopia may turn out to be a chancre on the cervix);
- blood for HIV infection and hepatitis;
- hormonal studies (according to indications);
- microflora smear.
Treatment of cervical ectopia
Treatment of cervical ectopia is carried out by a gynecologist.
If sexually transmitted infections are discovered during the examination, then the necessary specific therapy is first carried out.
Before treating pseudo-erosion, anti-inflammatory suppositories are prescribed for preventive purposes in short courses (for 3-5 days), for example, Polygynax or Betadine. Ectopic therapy is prescribed on days 5-7 of the menstrual cycle.
There are several treatment methods, each of which has its own advantages and disadvantages:
1. Chemical coagulation.
This method is conservative. The essence of chemical coagulation is to treat the pathological lesion with a mixture of acids (solkovagin), which cause a burn and the formation of a scab.
The advantages of chemical coagulation include complete or almost complete painlessness, low cost, possibility of use in nulliparous women, and ease of use.
The disadvantages of the method include frequent relapses of the disease and the inability to cauterize large erosions.
2. Laser treatment.
The affected area is treated with a laser beam, under the influence of which the liquid evaporates from the pathological cells and they are destroyed.
The advantages of laser vaporization are painlessness, complete cure (exclusion of relapses), rapid regeneration of the cervix without scar formation. In addition, after laser therapy there are practically no complications, the method can be recommended for nulliparous women.
Disadvantages include the high cost of using a laser and the need for special equipment.
3. Method of radio wave surgery (using the Surgitron apparatus).
Electrical waves are converted into radio waves, which, when entering soft tissues, lead to the evaporation of fluid from pathological cells and their destruction.
The advantages of the method include the absence of pain during treatment and healing of the cervix, an accelerated recovery process without the formation of scars and scabs, and the possibility of use in nulliparous patients.
The disadvantages of the method include the absence of the Surgitron device in some antenatal clinics.
Cryodestruction.
The essence of the method is to treat the cervix with liquid nitrogen: the pathological cells are frozen, crystals are formed in them, which lead to cell destruction and necrosis.
The advantages of cryodestruction include painlessness, the possibility of treating ectopia in nulliparous women, and bloodlessness.
Disadvantages of the method: the possibility of relapse, the appearance of bloody discharge in the postoperative period, the impossibility of treating extensive erosions.
4. Diathermocoagulation.
Diathermocoagulation is the treatment of the cervix with electric current, followed by the formation of a scab. The method is practically not used at present due to significant disadvantages: cicatricial deformation of the cervix, high risk of complications during and after surgery, prolonged healing, pain, and inability to use in nulliparous women. Of the advantages, only one can be named: the permissibility of using an electric knife to carry out conization of the cervix (the procedure for taking a small area of the uterus for further research).
After treating ectopia in one way or another, wound-healing suppositories and tampons (with levomekol, methyluracil) are prescribed for 7-10 days.
Consequences and prognosis
If erosion is left untreated for a long time, it can turn into cervical cancer. In addition, untreated ectopia promotes infections.
The prognosis is favorable.
- This is a fairly common phenomenon among women of childbearing age. Sometimes ectopia is called cervical erosion.
But this name is not only alarming, but also misleading. This is not cancer or disease. However, this phenomenon can create problems for some women.
What is cervical ectopia?
(syn.: erosion, pseudo-erosion, false, ectropion) is a condition in which a fragment of the single-layer glandular epithelium of the cervical canal covers the vaginal part of the cervix.
When examined, this area looks like a red spot, so many gynecologists quite often mistake ectopia for true erosion. Unlike erosion, the ectopic fragment does not bleed, since there is no defect in the mucous membrane.
Normally, the vaginal part of the cervix is covered with stratified squamous epithelium. The area where the two types of epithelium meet is called the transformation zone.
Columnar epithelium is thinner, therefore, in the transformation zone with stratified squamous epithelium, the appearance of a defect in the cervical tissue is created and an incorrect diagnosis can be made, which affects further erroneous treatment tactics.

What is the danger of ectopia?
Ectopia itself is not dangerous, but its morphological picture is very similar to the first and second stage of cervical cancer.
To perform laser destruction, general anesthesia is required.
The procedure is carried out by directing a carbon dioxide laser beam to the affected areas of the cervix. Healthy tissues remain untouched when exposed to laser.
Advantages of the method:
- accuracy of tissue cauterization;
- absence of infectious complications, bleeding;
- rapid wound healing within 4 weeks.
There is only one drawback - the high cost of the equipment and the procedure itself.
Radiosurgery
Radio wave treatment is effective and safe. The method is accurate, healthy cells remain unchanged. This type of treatment is absolutely painless and leaves no scars.
This method of removing abnormal cervical tissue is performed using a thin wire loop that has a low voltage electric current.
The procedure takes only a few minutes. It may be followed by mild cramping for several hours and dark brown vaginal discharge for the first week.
Radiosurgery is more gentle than carbon dioxide laser treatment.

Thermocoagulation
Synonym: diathermocoagulation- a method in which erosion will be cauterized by applying high temperature to the desired affected area. Under the influence of heat, the columnar epithelium is destroyed and the exposed area of the cervical canal is subsequently covered with stratified squamous epithelium.
Diathermy destroys the entire infection lying in the depths of the glandular epithelium, so purulent complications rarely occur. requires dilation of the cervical canal and general anesthesia or local anesthesia; otherwise, cervical stenosis may occur.
Indications:
- cervicitis;
- precancerous diseases of the cervix;
- bleeding.
Progress of the procedure:

Thermocoagulation gives satisfactory treatment results, but has strengths and weaknesses.
Advantages of the method:
- precise control of the procedure;
- good hemostasis;
- availability and relative cheapness.
Flaws:
- several procedures may be required;
- pain during manipulation;
- outdated method;
- not suitable for women planning to become pregnant.
Surgical methods
The most common surgical method for treating dysplasia or cervicitis is conization of the cervix. This operation is used if all of the above treatment methods are ineffective or if the lesion is large.
Conization is performed under general anesthesia using a laser or a cold knife.
 The essence of the operation:
The essence of the operation:
- Cone-shaped resection (removal) of the cervix.
- Preliminary expansion of the cervical canal ensures the prevention of postoperative stenosis.
- After the operation, antibacterial drugs are prescribed, and sexual abstinence is recommended for 6-8 weeks.
Possible long-term postoperative complications:
- premature birth;
- spontaneous abortion;
- isthmic-cervical insufficiency.
Chemical coagulation
Chemical cauterization is a safe method.
Progress of the procedure:

Advantages of the method:
- simplicity of the procedure;
- cheapness;
- healthy cells are not exposed to chemical effects.
Flaws:
- chemical coagulation is effective only in case of a small affected area;
- the effect of the procedure can be observed only after a few days.
Traditional methods
Treatment with traditional methods consists of taking decoctions based on leaves and flowers of plants and fruits:

Postoperative treatment
In the postoperative period, analgesics and antibiotics are prescribed if necessary.
Precautions after intervention
If the following symptoms appear, consult a doctor immediately:
- foul-smelling vaginal discharge;
- heavy bleeding;
- more than 4 weeks;
Prevention
Prevention measures:
- To prevent the occurrence of cervical ectopia, you must remember to undergo preventive examination by a gynecologist once a year.
- And also important treat all sexually transmitted infections in a timely manner, inflammatory processes.
- Sexual intercourse should always be protected to prevent the development of various diseases.
- When diagnosing cervical ectopia, it is necessary to attend annual examinations with mandatory colposcopy and cytology to avoid the development of a malignant tumor.
- Psychologists have conducted many studies, as a result of which they found that most often ectropion and erosion develop in women who are dissatisfied with themselves.
Ectopia is not dangerous for a woman only if it is diagnosed in a timely manner. In case of the slightest changes in the cells of the cervical canal, timely treatment must be started.
Forecast
The prognosis is favorable with the correct treatment method:
- Electrosurgery has a fairly high level of effectiveness, the relapse rate after cauterization ranges from 2% to 15%.
- Chemical coagulation effective only for mild dysplasia.
- Laser vaporization ia in second place in terms of treatment results after electrosurgery, the incidence of relapses is from 3% to 24%.
Conclusion
 Cervical ectropion in gynecology is considered a benign condition and not a disease.
Cervical ectropion in gynecology is considered a benign condition and not a disease.
Many nulliparous women do not even suspect that they have ectopia until it is discovered during a routine examination.
Pregnant patients are not treated with treatment, as it can harm pregnancy and childbirth.
Only a doctor can diagnose ectropion.
If you are concerned about symptoms such as bleeding or heavy vaginal discharge, you should immediately undergo an examination. Since a number of conditions can imitate other diseases - sexually transmitted infections, cervical cancer.
No one will take better care of our health than ourselves.
- (from the Greek ektopos displaced) congenital or acquired displacement of an internal organ or tissue, sometimes with access to the surface of the body (for example, ectopia of the bladder) ... Big Encyclopedic Dictionary
ECTOPY- (ectopia), a term used in pathology to designate certain cases of prolapse, outward displacement of organs and tissues. E. can be either congenital due to developmental defects or acquired. Examples may be: E. bladder... ... Great Medical Encyclopedia
Noun, number of synonyms: 1 offset (44) ASIS synonym dictionary. V.N. Trishin. 2013… Synonym dictionary
ectopia- and, f. ectopie f., German Ektopie gr. ektopos moved. honey. Abnormal displacement of what n. organ. Krysin 1998. Lex. SIS 1954: ecto/pia; SIS 1964: ectopic/i... Historical Dictionary of Gallicisms of the Russian Language
ectopia- Congenital movement of internal organs (or tissues) to an unusual location, often closer to the surface of the body, for example, movement of the heart to the cervical region, etc. [Arefyev V.A., Lisovenko L.A. English-Russian explanatory dictionary of genetic terms 1995 ... Technical Translator's Guide
- (from the Greek ektopos displaced), congenital or acquired displacement of an internal organ or tissue, sometimes with access to the surface of the body (for example, ectopia of the bladder). * * * ECTOPIA ECTOPIA (from the Greek ektopos displaced), congenital or... ... encyclopedic Dictionary

